7 Clear Differences Between Type 1 and Type 2 Diabetes: Understand the Key Distinctions
Introduction: Understanding Type 1 and Type 2 Diabetes
Diabetes is a condition that affects millions worldwide, but many people still find it difficult to distinguish between the different types. While Type 1 and Type 2 diabetes share similarities, they also have distinct characteristics that impact how they are managed and treated. In this blog post, we will break down 7 clear differences between Type 1 and Type 2 diabetes to help you better understand each condition, their causes, symptoms, treatments, and how they affect the body.
1. Cause of the Condition
The root cause of diabetes largely determines its type. Here’s how:
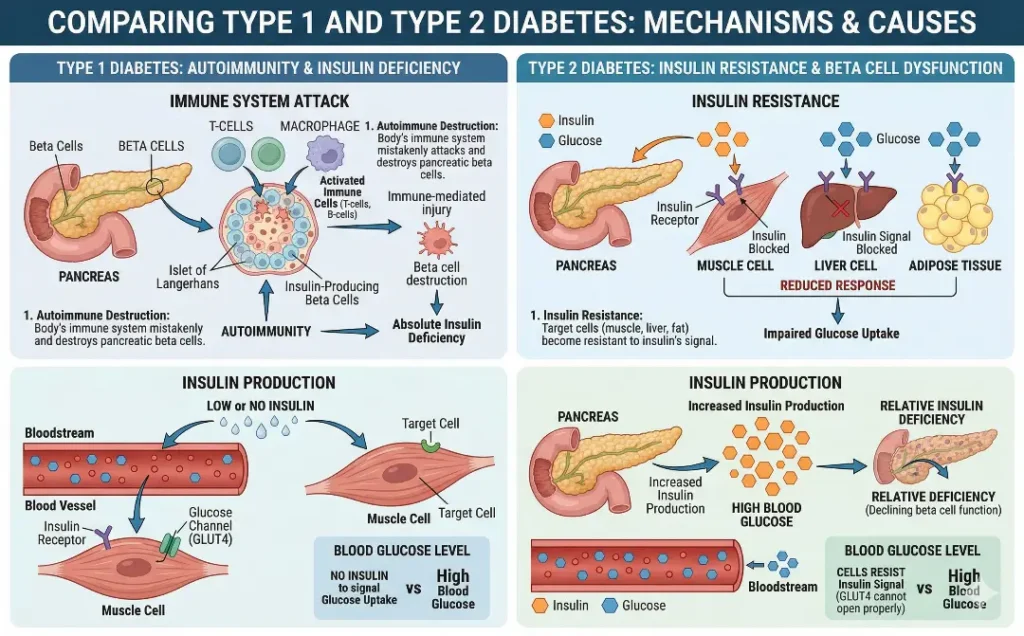
- Type 1 Diabetes: This type is an autoimmune disorder where the body’s immune system mistakenly attacks and destroys the insulin-producing beta cells in the pancreas. This results in little to no insulin production, leaving the body unable to regulate blood sugar levels. Type 1 diabetes typically develops in childhood or early adulthood.
- Type 2 Diabetes: Unlike Type 1, Type 2 diabetes is caused by insulin resistance. In this case, the body still produces insulin, but the cells do not respond to it effectively. Over time, the pancreas cannot produce enough insulin to maintain normal blood sugar levels. Type 2 diabetes is more common in adults, although it is increasingly being diagnosed in children due to rising obesity rates.
2. Age of Onset
One of the easiest ways to distinguish between Type 1 and Type 2 diabetes is the age at which they typically develop:
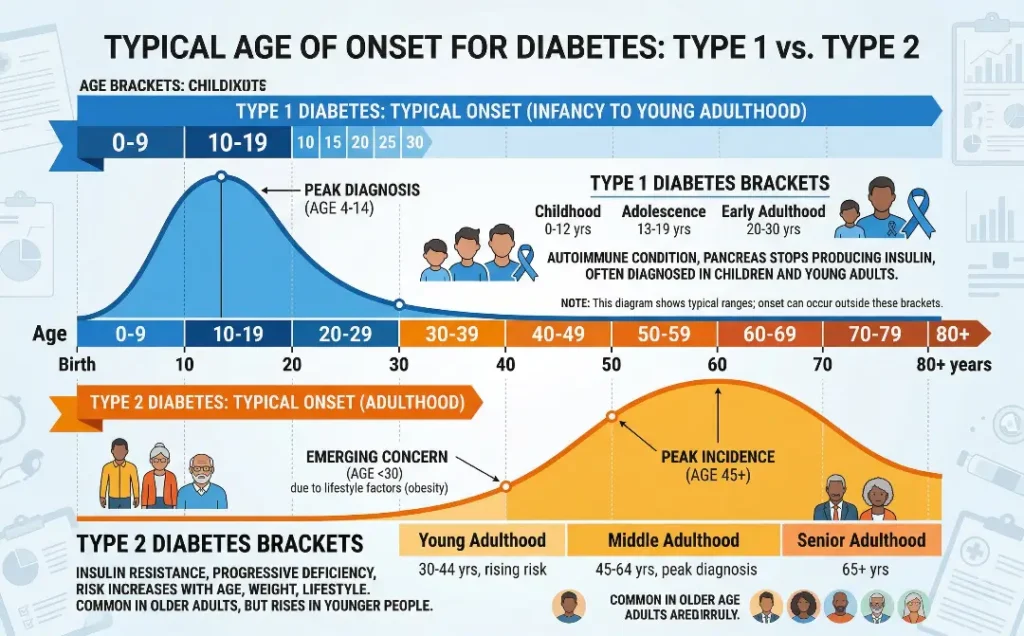
- Type 1 Diabetes: Usually diagnosed in children, teenagers, or young adults. It often appears suddenly and can worsen quickly.
- Type 2 Diabetes: Generally develops in adults over the age of 45, although it can be seen in younger individuals, especially those who are overweight or have a family history of diabetes.
3. Symptoms at the Time of Diagnosis
While both types of diabetes share some common symptoms, the onset and severity can differ significantly:
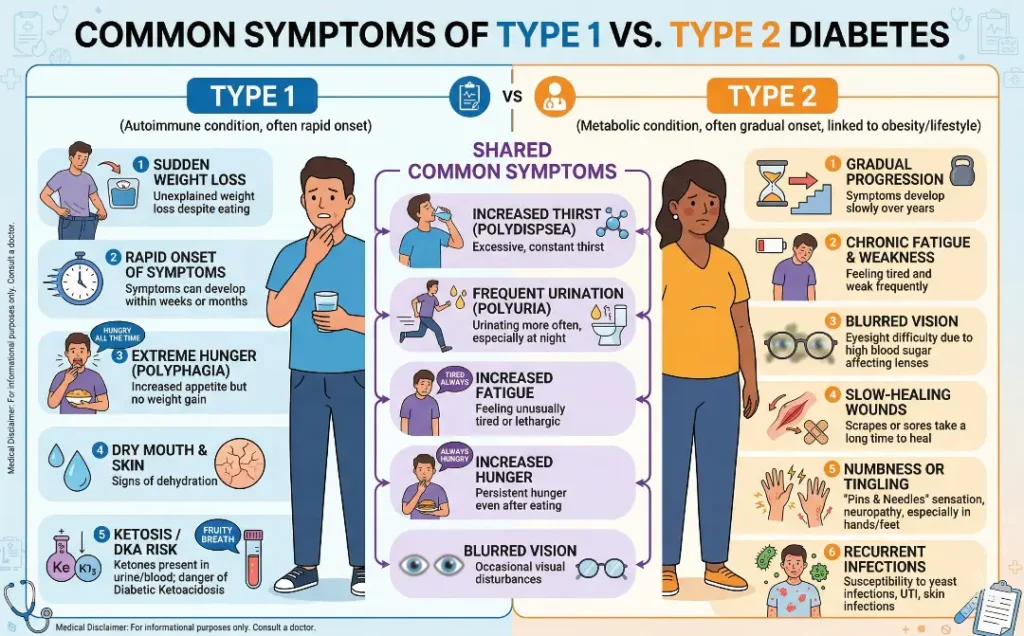
- Type 1 Diabetes: Symptoms tend to appear suddenly and may include extreme thirst, frequent urination, unintentional weight loss, fatigue, blurred vision, and nausea. If not treated promptly, it can lead to a diabetic coma.
- Type 2 Diabetes: Symptoms develop gradually over time, and many people may not experience noticeable symptoms in the early stages. Common symptoms include increased thirst, frequent urination, unexplained weight loss, slow-healing sores, and tingling or numbness in the hands or feet.
4. Treatment Approaches
The treatment for each type of diabetes is distinct due to the different underlying causes:
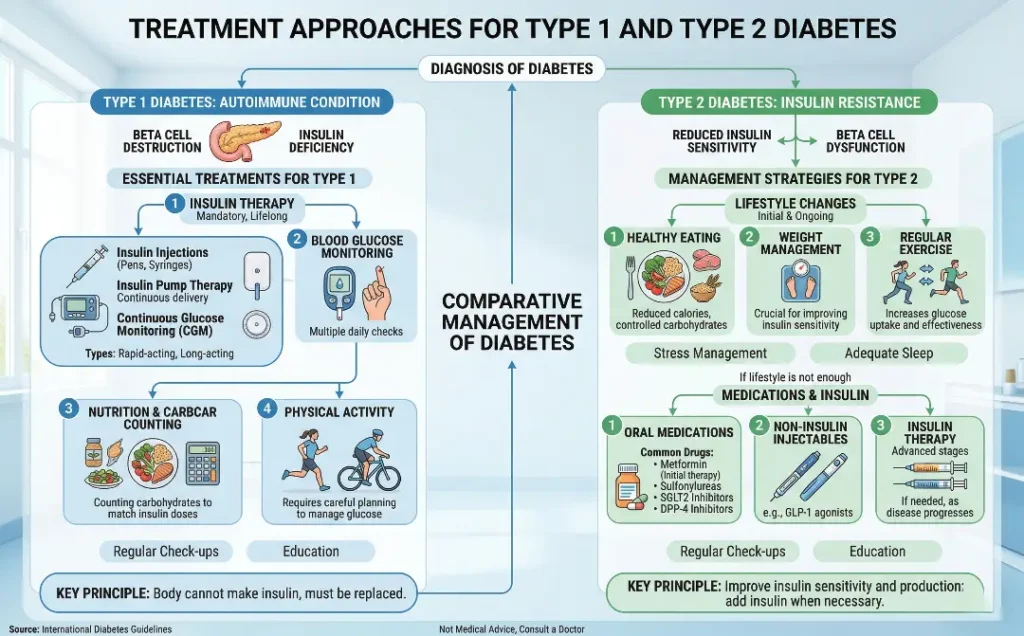
- Type 1 Diabetes: Insulin therapy is the main treatment for Type 1 diabetes. People with Type 1 need to inject insulin daily or use an insulin pump to manage their blood sugar levels. Other treatments include carbohydrate counting, exercise, and blood glucose monitoring.
- Type 2 Diabetes: Initially, Type 2 diabetes may be managed with lifestyle changes such as diet and exercise. However, medications, including oral drugs like metformin, may be prescribed to help the body use insulin more effectively. In some cases, insulin therapy may also be required if the disease progresses.
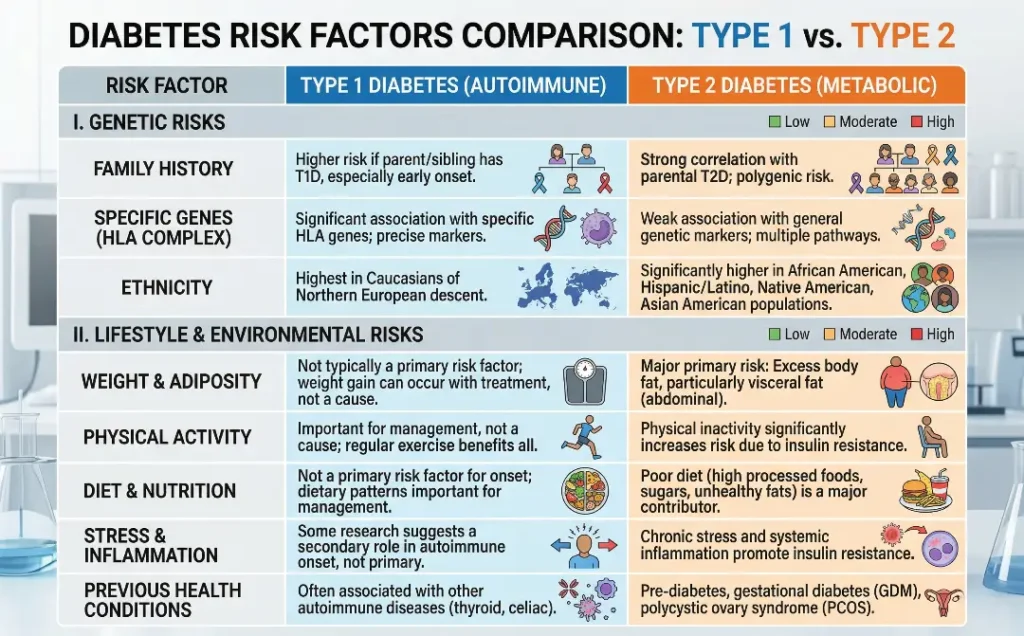
5. Risk Factors
Certain factors increase the risk of developing each type of diabetes:
- Type 1 Diabetes: The exact cause is unknown, but genetics and family history play a role. Type 1 diabetes is more common in people with a family history of autoimmune diseases.
- Type 2 Diabetes: Several factors contribute to the development of Type 2 diabetes, including being overweight, having a sedentary lifestyle, poor diet, high blood pressure, and a family history of diabetes. Age, ethnicity, and certain medical conditions like polycystic ovary syndrome (PCOS) also increase the risk.
6. Prevention and Management
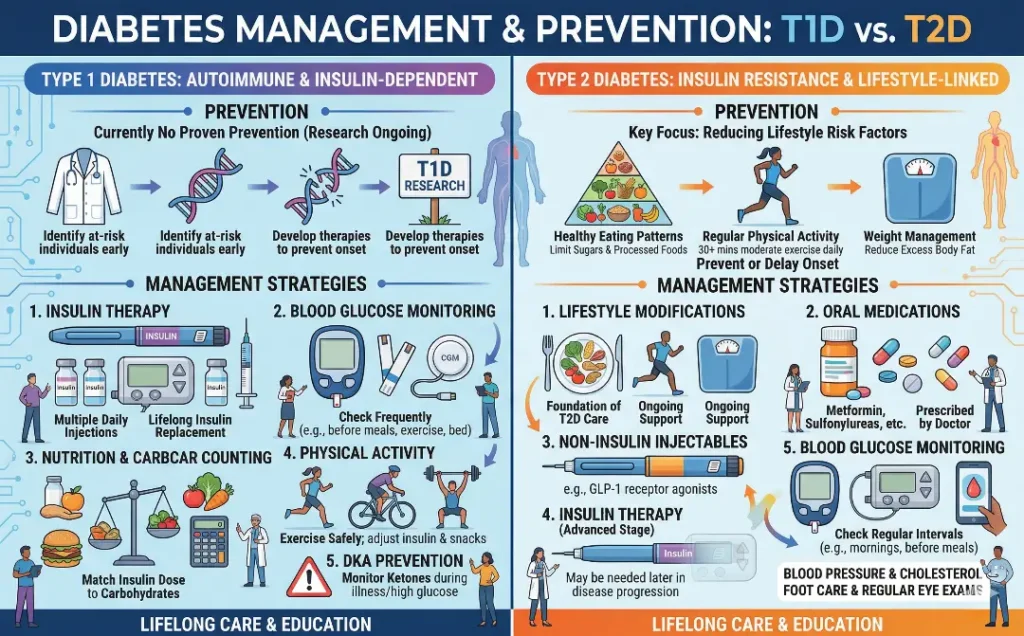
Prevention and management differ significantly between the two types of diabetes:
- Type 1 Diabetes: Since Type 1 diabetes is an autoimmune condition, it is not preventable. Management primarily focuses on maintaining blood sugar levels through insulin therapy, diet, and regular exercise.
- Type 2 Diabetes: Type 2 diabetes is preventable in many cases through lifestyle changes such as maintaining a healthy weight, eating a balanced diet, and staying active. Early detection and intervention can often delay or even prevent the onset of the condition.
7. Impact on the Body Over Time
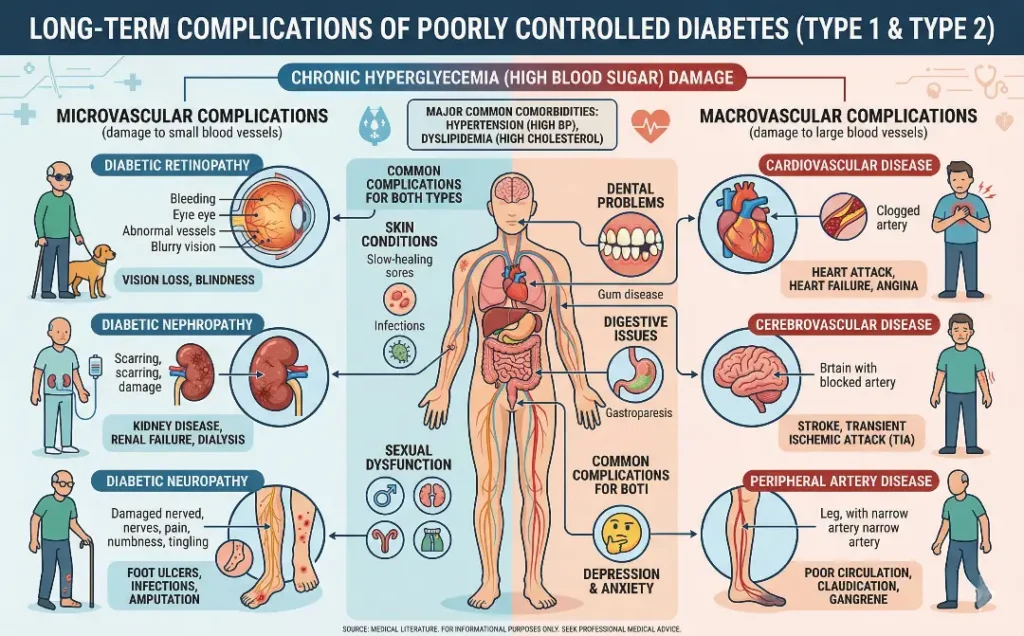
The long-term effects of Type 1 and Type 2 diabetes on the body can vary, but both types can cause serious health complications if not properly managed:
- Type 1 Diabetes: People with Type 1 diabetes are at risk for complications such as diabetic ketoacidosis (a potentially life-threatening condition), heart disease, nerve damage, and kidney failure.
- Type 2 Diabetes: Over time, poorly controlled Type 2 diabetes can also lead to serious complications like heart disease, stroke, nerve damage, kidney disease, and vision problems. However, these complications are often preventable with effective blood sugar control and healthy lifestyle choices.
Conclusion: Key Takeaways
Understanding the 7 clear differences between Type 1 and Type 2 diabetes is crucial for anyone living with or at risk for the condition. While they share some similarities, their causes, symptoms, and treatment approaches are unique. Whether you are dealing with diabetes or just seeking more knowledge about the condition, knowing these key differences will help you better manage the disease and take the necessary steps toward prevention.
Remember, with early intervention and proper management, both Type 1 and Type 2 diabetes can be controlled, allowing individuals to lead healthy, active lives.
By breaking down the 7 clear differences between Type 1 and Type 2 diabetes, we’ve provided a detailed comparison that will hopefully give you a better understanding of these two conditions. Always consult with a healthcare professional for a tailored approach to managing your health.
